Dental implant screw: uses & placement procedure
Dental implants have revolutionized the way we approach missing teeth, offering a durable and aesthetically pleasing solution.
At the heart of this dental innovation are dental screws, small but critical components that play a pivotal role in the success of dental implants. These screws, technically known as implant fixtures, serve as the anchor for the artificial tooth, providing stability and support that mimics the root of a natural tooth. Understanding how dental screws work within the context of dental implants is essential for anyone considering this form of dental restoration. Read this quick guide to learn more!
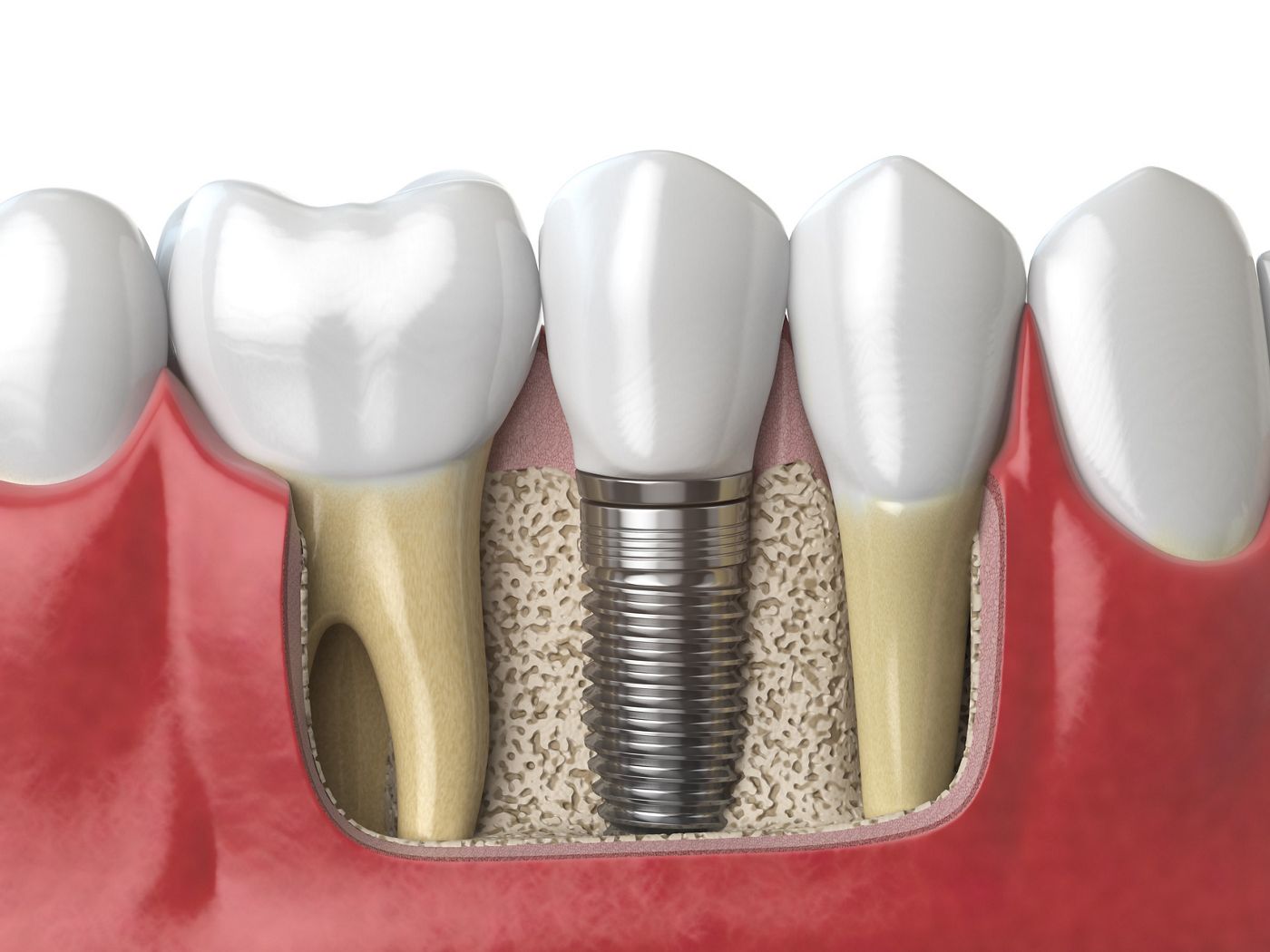
What is the purpose of dental screws in dental implants?
Dental screws are designed to integrate with the jawbone in a process known as osseointegration. This integration provides a stable foundation for the dental implant, ensuring that the artificial tooth remains securely in place.
The primary purpose of dental screws is to replicate the function of a natural tooth's root, absorbing and distributing the forces generated during chewing. By doing so, dental screws help maintain the integrity of the jawbone, preventing bone loss that often accompanies tooth loss.
What are dental screws?
Dental screws, or implant fixtures, are small titanium posts that are surgically placed into the jawbone. Titanium is chosen for its biocompatibility, allowing the body to accept and integrate with the metal without adverse reactions.
These screws come in various sizes and shapes, tailored to fit the specific anatomical requirements of the patient's jawbone and the type of implant being used. Dental screws act as the foundation for the rest of the implant structure, which includes the implant abutment (the connector piece) and the dental prosthesis (the visible tooth replacement which is made to blend in with natural teeth).
What material are dental screws made of?
Most dental screws are made from titanium because of its strength, durability, and compatibility with human biology. Titanium's unique ability to fuse with bone through osseointegration is what makes it the material of choice for dental implants. However, in some cases, zirconia, a type of ceramic, is also used.
Zirconia offers an aesthetic advantage with its tooth-like colour, making it an excellent option for patients with metal sensitivities or for implants in the front of the mouth where a metal implant might be more visible, commonly for dental implant procedures for the front teeth.
Where exactly are dental screws placed?
Dental screws are placed directly into the jawbone at the site of the missing tooth. The placement procedure involves drilling a small hole into the bone, into which the dental screw is then inserted.
The location and angle of placement are carefully planned to maximize contact with the bone and to avoid damaging any vital structures such as nerves or sinuses. This strategic placement is crucial for the stability of the implant and its ability to support the forces of biting and chewing.
Why are dental screws important in dental implants?
The importance of dental screws in dental implants cannot be overstated. They are the foundation upon which the entire implant structure is built. Without the stability provided by the dental screw, the artificial tooth would not be able to withstand the daily forces exerted upon it.
Furthermore, dental screws stimulate bone growth around the implant, a critical factor in preventing bone loss and maintaining the facial structure. Their role in promoting osseointegration ensures the longevity and success of the retained screw dental implant.
How long do dental screws last?
With proper care and maintenance, dental screws can last a lifetime. The success rate of dental implants is high, with studies showing long-term success rates of over 95%.
Factors that can affect the longevity of dental screws include the patient's oral hygiene, dental care, lifestyle habits, and the presence of any underlying health conditions that may impact bone health.
Regular dental check-ups and cleanings are essential to monitor the health of the implant and to address any issues that may arise.
Can dental implant screws fall out?
While dental implants are designed to be a long-term solution for missing tooth or teeth, there are rare instances where the screw can fail and become loose or fall out due to the screw loosening.
This can happen due to several reasons, such as improper osseointegration (the process by which the implant integrates with the bone), infection, gum disease, excessive force on the implant, or inadequate oral hygiene for teeth and gum maintenance.
However, with proper planning, surgical techniques used in the dental clinic chosen, and post-operative care, the risk of implant failure is low. Regular dental check-ups and maintaining good oral hygiene can significantly reduce the risk of implant failure.